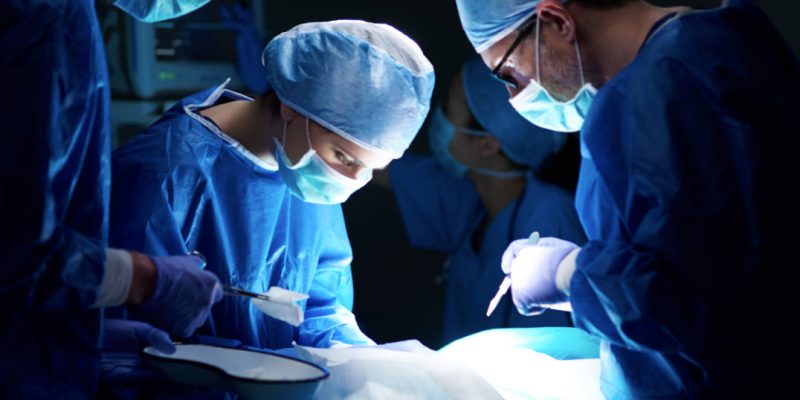
Defective medical devices can turn trust into harm. You expect a device to heal, not to cause new pain, infection, or disability. Yet pacemakers can fail, joint implants can break, and surgical mesh can tear. Each failure can change your life in one moment. This blog explains what you need to watch for, how to protect yourself, and when to speak up. You will learn common warning signs, steps to take after a device problem, and how doctors, hospitals, and companies share responsibility. You will also see how product liability claims work when a device is unsafe. The goal is simple. You deserve clear facts, not confusion. You deserve safe care, not excuses. When you understand the risks, you can ask better questions, push for answers, and stand firm if something feels wrong.
What counts as a medical device
You meet medical devices in daily life. Some sit on your skin. Others sit inside your body.
- At home. Blood pressure cuffs. Glucose meters. Home EKG devices.
- In a clinic. Infusion pumps. Monitors. Surgical tools.
- Inside your body. Pacemakers. Stents. Joint implants. Mesh. Pumps.
The U.S. Food and Drug Administration explains that a medical device is any tool or machine used to diagnose, treat, or prevent disease. It can be simple or complex. It can be temporary or permanent. You can read more on the FDA medical device overview page.
How devices fail and why it matters
A device can fail in three main ways.
- Design flaws. The product is unsafe even when used as directed.
- Manufacturing defects. Some units leave the factory with hidden problems.
- Warning problems. Instructions and labels leave out key risks.
When a device fails, the result is not a small nuisance. It can cause bleeding. It can trigger infection. It can damage organs. It can even cause death. You may need more surgery. You may lose income. Your family may carry new stress and fear.
Common warning signs something is wrong
Trust your body. If you have an implanted or regular use device, watch for changes like these.
- New or rising pain near the device site
- Redness, warmth, or drainage from an incision
- Sudden swelling or hard lumps
- Shocks, fluttering, or skipped beats with heart devices
- Unusual alarms or error messages on pumps or monitors
- Device not turning on, holding charge, or working as before
- Fainting, shortness of breath, or chest discomfort
Do not wait and hope it passes. First call your doctor or device clinic. If you have chest pain, trouble breathing, or fast bleeding, call emergency services right away.
Recalls, safety alerts, and what they mean for you
The FDA tracks problems and issues recalls and safety alerts. A recall does not always mean you must remove the device. Sometimes it means a software update. Sometimes it means a change in instructions. Other times it may mean surgery.
Types of FDA device actions and what they usually mean
| Type of action | What it usually means | What you should do |
|---|---|---|
| Safety communication | FDA shares new risk information | Read trusted sources. Talk with your doctor. Do not stop using a device on your own. |
| Class III recall | Low chance of harm | Follow new instructions. Ask if any change in your care is needed. |
| Class II recall | Possible temporary or reversible harm | Call your doctor. Ask if repair, update, or close watch is needed. |
| Class I recall | Risk of serious harm or death | Contact your care team at once. Ask about urgent steps, including replacement. |
You can search current device recalls on the FDA medical device recall database. Check this site if you hear about a recall on the news or from other patients.
How to protect yourself before you get a device
You cannot remove all risk. Yet you can lower it. Use three simple steps.
- Ask clear questions. What device will you get. How long has it been in use. What problems have been reported. What other options exist.
- Check the record. Ask if the device has a black box warning, ongoing recall, or many past complaints.
- Understand the plan. Ask how follow up will work. Ask what symptoms should trigger a call or visit.
Write questions down before your visit. Bring a family member to help listen and take notes.
Steps to take if you suspect a defect
If you think your device is failing, act in three stages.
- First protect your health. Get medical care. Tell providers about the device and symptoms.
- Then protect evidence. Keep device cards, manuals, packaging, and receipts. If a device is removed, ask that it be saved if possible.
- Finally report the problem. Ask your doctor to report to the FDA. You can also file a report yourself through the FDA MedWatch system on the same recall site.
Who may be responsible
Responsibility can rest with several groups.
- The company that designed or made the device
- The distributor that stored or shipped it
- The hospital or clinic that used or implanted it
- The provider who chose or placed it in an unsafe way
In some cases, injured patients use product liability claims to seek payment for medical bills, lost income, and pain. Talking with a qualified lawyer can help you understand if that path fits your case.
How to speak up and still feel safe
Many patients stay silent because they fear blame. You may worry that your doctor will be angry. You may feel shame about complaining. Your fear is real. Yet your safety must come first.
- Use simple words. Say “I am worried this device is hurting me.”
- Stay focused on facts. Describe when symptoms started and how they changed.
- Bring someone you trust. Another set of ears can help keep the talk calm.
If you feel dismissed, you can ask for a second opinion. You have that right. Your body and your story matter.
Key takeaways for you and your family
Defective medical devices can cause long lasting damage. Yet you are not powerless. You can learn about the device you use. You can watch for warning signs. You can report problems. You can ask hard questions about safety and recalls.
When something feels wrong, treat that feeling as a warning. Speak up early. Seek care fast. Demand clear answers. Your voice can protect your health. It can also protect other patients who may face the same hidden risk.